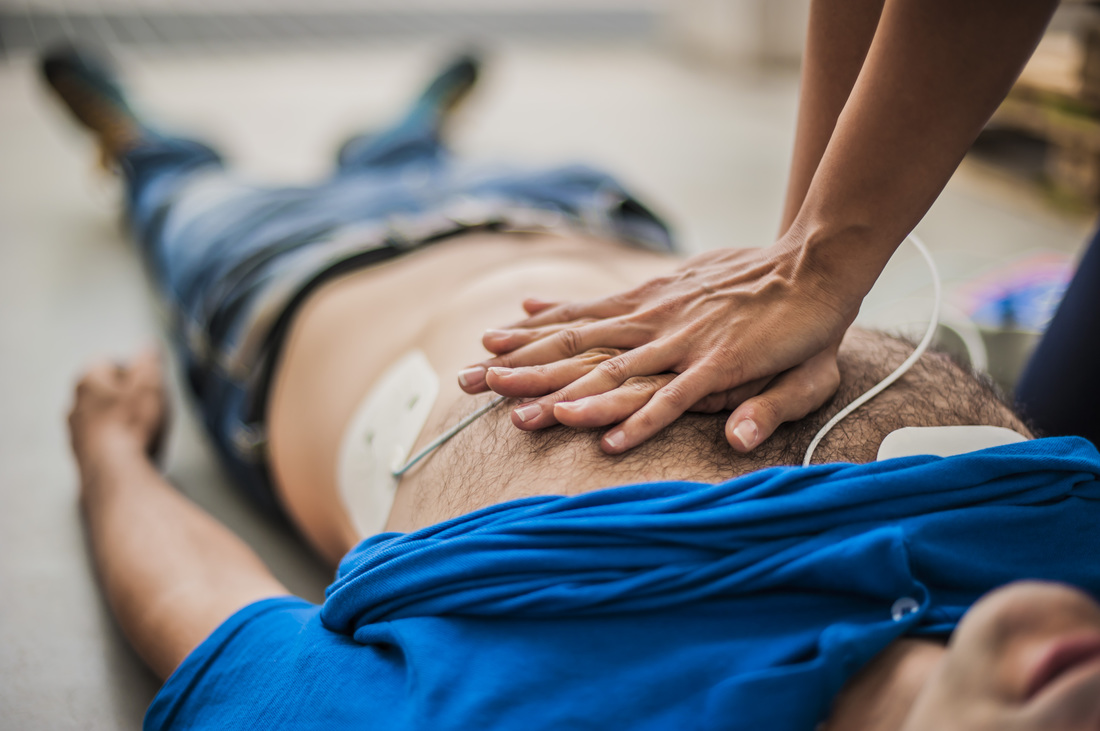
Training more community members, patients and families to recognize and respond to a cardiac arrest before medical help arrives may help more victims survive, a U.S. study suggests.
Cardiac arrest often proves fatal when it happens outside a hospital because bystanders don’t know how to start chest compressions or use an external defibrillator to keep the patient’s blood flowing to vital organs until emergency responders reach the scene.
“Every minute counts; therefore, effective and prompt bystander CPR is critical and (is) the first link after activating EMS by calling 911,” said lead study author Dr. Christopher Fordyce of Vancouver General Hospital and the University of British Columbia in Canada.
For the study, researchers examined survival odds in North Carolina after a statewide program was initiated in 2010 to train community members, patients with heart disease and their families to do chest compressions. Among other things, the program also trained school staff to use automated external defibrillators (AEDs) and taught emergency medical dispatchers how to instruct bystanders in cardiopulmonary resuscitation (CPR)
Over five years, the proportion of patients receiving bystander CPR climbed from 28 percent to 41 percent for home-based cardiac arrests and from 61 percent to 72 percent for those that happened in public. The proportion of patients receiving defibrillation at home also increased from 42 percent to 51 percent.
At the same time, the proportion of people who had a cardiac arrest at home and lived long enough to leave the hospital rose from 5.7 percent to 8.1 percent, while survival odds for a cardiac arrest in public increased from 10.8 percent to 16.2 percent. The North Carolina project was funded by $2.5 million over five years from the Medtronic Foundation, Fordyce said by email.
“I would say that at $500,000 a year this is fairly cost-effective for a statewide initiative that improved care processes and saved lives,” Fordyce said.
Cardiac arrest involves the abrupt loss of heart function, breathing and consciousness. Unlike a heart attack, which happens when blood flow to a portion of the heart is blocked, cardiac arrest occurs when the heart’s electrical system malfunctions, often due to irregular heart rhythms. Cardiac arrest may occur with no warning and is often fatal.
When patients had a cardiac arrest at home, survival odds were 55 percent higher if they received CPR from a bystander and defibrillation from EMS than if they didn’t receive CPR before medical help arrived, researchers report in JAMA Cardiology.
In public, cardiac arrest survival odds were more than quadrupled when patients had both CPR and defibrillation administered by a bystander than when they waited for EMS to arrive, the study also found.
The study included data on 5,602 people who had a cardiac arrest at home and another 2,667 who had a cardiac arrest in public in 16 North Carolina counties over five years. Combined, these counties have about 3.3 million residents and included both urban and rural areas.
It wasn’t a controlled experiment designed to prove that the training program directly saved lives.
Survival odds improved, but remained low, based on how many people lived long enough to leave the hospital, and the study also lacked longer-term survival data, the authors note.
Even so, the results suggest that efforts to get more bystanders involved can make a difference, said Dr. Graham Nichol, co-author of an accompanying editorial and director of the University of Washington-Harborview Center for Prehospital Emergency Care in Seattle.
“In many communities, survival after out-of-hospital cardiac arrest has been static for decades,” Nichol told Reuters Health by email. “This work showed that implementing a bundle of education strategies improved outcomes; the sum appeared greater than the parts.”
Earlier bystander intervention can also help preserve brain function in patients who survive, said Dr. Lenworth Jacobs, a researcher at the University of Connecticut and director of the Trauma Institute at Hartford Hospital.
“This is an issue of seconds and minutes,” Jacobs, who wasn’t involved in the study, said by email. “Three or four minutes can make a dramatic difference in the functional outcome and survival of these patients.”